On the 21st September The United Nations General Assembly held a meeting on the issue of antibiotic resistance and it’s not a moment too soon.
Imagine a time when cancer treatment and organ transplants are impossible, open-heart surgery and hip replacements are high risk and rarely carried out, women die in childbirth and deaths from pneumonia and STIs are common. I doubt many of you thought of the future, but if antibiotic resistance continues at its current rate – it could be. Already more than 700,000 people a year die from drug resistant infections; in 2050 it could be as many as 10 million (which is more than the number of people who die from cancer at the moment). Not only will we lose modern medicine to antibiotic resistance, it will also cost the economy $100 trillion between now and 2050, with annual costs as large as those caused by the financial crisis of 2008.
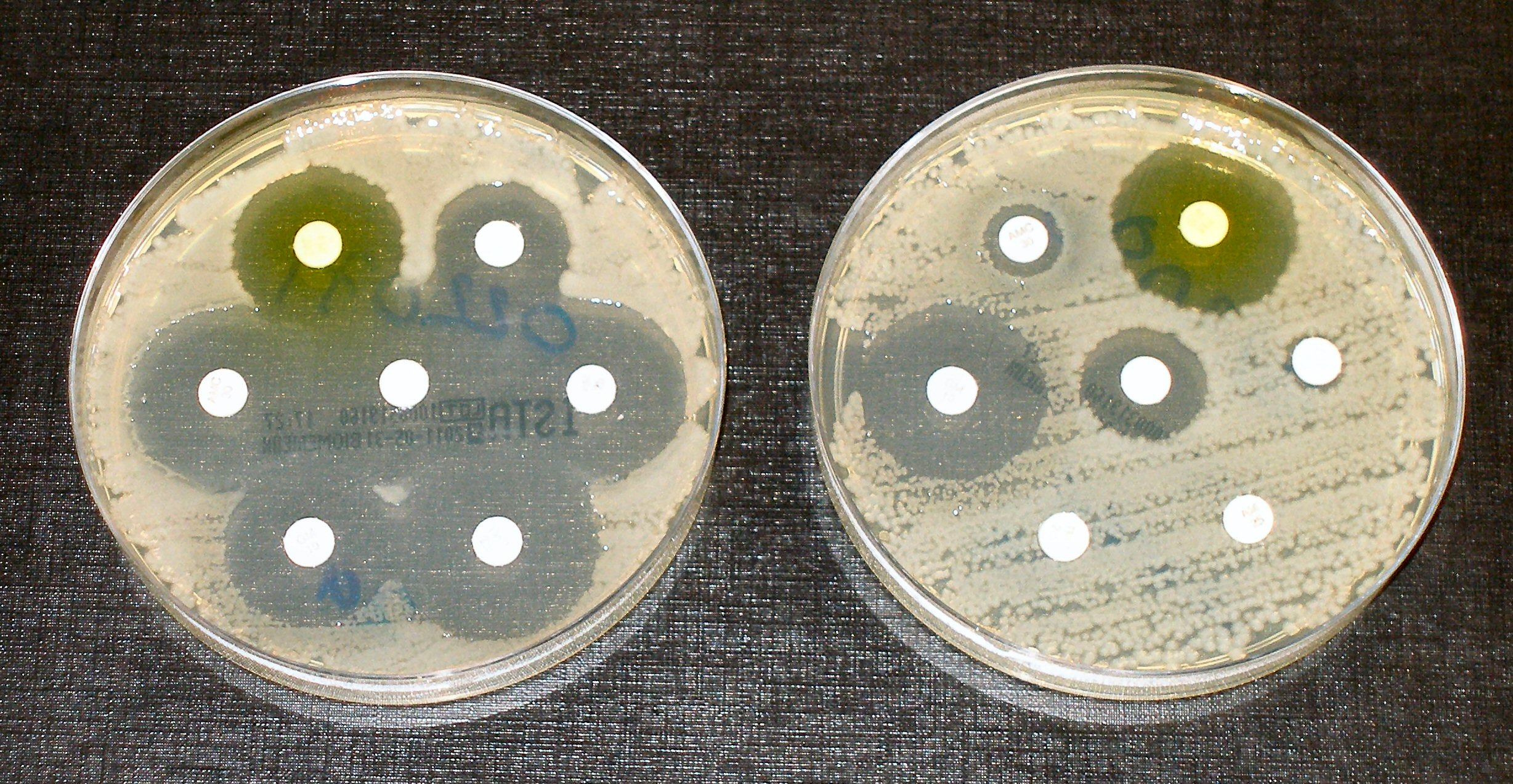
To understand how we got to this point, a brief lesson in biology is required. Amongst any population, including that of bacteria, there is genetic variation or mutations. In the case of bacteria some of these mutations will code for resistance to antibiotics. If this population is exposed to antibiotics then only bacteria with the antibiotic resistance gene will survive and reproduce, forming a bacterial strain that is resistant to said antibiotic. The problem we are now facing is that more populations of bacteria are being exposed to more antibiotics, making antibiotic resistant strains more common and resistant to more than one class of antibiotic.
“Only 2 new classes of antibiotic have been developed in the last 40 years”
One of the main reasons that antibiotic resistance is increasing at such a rapid rate is widespread use of antibiotics by people who might not need them. In 2012 antibiotic prescriptions reached an all-time high with 3.8 million prescriptions being given out. Over-worked GPs often end up prescribing antibiotics for symptoms caused by viruses like sore throats, as it’s quicker than explaining to the patient that an antibiotic will not cure such symptoms. However GPs who take the time to educate their patients save themselves time in the long run as the same patient is less likely to make appointments for the same illness in the following year. Doctors have a second problem in that there’s no readily available test to assess whether symptoms are being caused by a bacterial infection or a virus so they have to rely on their own judgment, this results in several prescriptions being made ‘just in case’.
On top of this antibiotics are used in similar quantities in agricultural livestock, exposing even more bacteria to antibiotics. Antibiotics are used to promote growth and fend off costly infections which are common in intensively farmed animals. Many of the antibiotics given to animals do not require a prescription from a vet so their usage is completely unregulated. This means that even antibiotics vital for human health as they can kill some of the most resistant strains of bacteria, are being used widely in farm animals. In the last year a strain of bacteria resistant to Colistin, a last resort drug, was identified in Chinese meat products. However this issue can’t be resolved as simply as banning all antibiotics in farming; though developed countries with stable food supplies may be able to cope, poorer countries will struggle to produce enough protein for their growing populations if antibiotic usage is heavily reduced.
Adding to the problem of antibiotic over-use is the fact that research in the field has been dwindling. Only 2 new classes of antibiotic have been developed in the last 40 years. Pharmaceutical companies have turned their backs on antibiotic development as it’s low profit and there is more money to be made out of illnesses like cancer and heart disease.
Fortunately these issues are finally being addressed as last month the United Nations General Assembly called a high level meeting on antibiotic resistance. Prior to this meeting only 3 others of this level have been held on health issues: HIV/AIDs, Ebola and non-communicable diseases. The 193 member states signed a declaration at the meeting resolving to combat proliferation of antibiotic resistance by encouraging innovation in antibiotic development ($72 million has already been contributed by the UK and China to the global innovation research fund to try and make this happen), increasing public awareness and regulating the use of antibiotics in humans and animals. It’s a good starting point and will provide advocates with the grounds to enforce change. Hopefully at the review in 2 years time, we’ll find that medicine is continuing to push forward, rather than heading for a gruesome return to the dark ages.
IMAGE: Wikimedia Commons